Hydration: A Subtle, Overlooked Risk Factor Most People Ignore
by Edison de Mello, MD, PhD
For decades, we have explained heart attacks through familiar risk factors: cholesterol, diet, smoking, stress, lack of exercise, and genetics. While all of these matter, they do not fully explain one striking and well-documented phenomenon: the majority of heart attacks and strokes occur in the early morning hours, most commonly between 5 a.m. and 10 a.m.
This pattern has been observed consistently across populations, countries, and decades. The question is not whether it happens, but why. The answer lies less in what we eat or how stressed we feel, and more in predictable physiological changes that occur every morning, often amplified by one simple, unconscious habit.
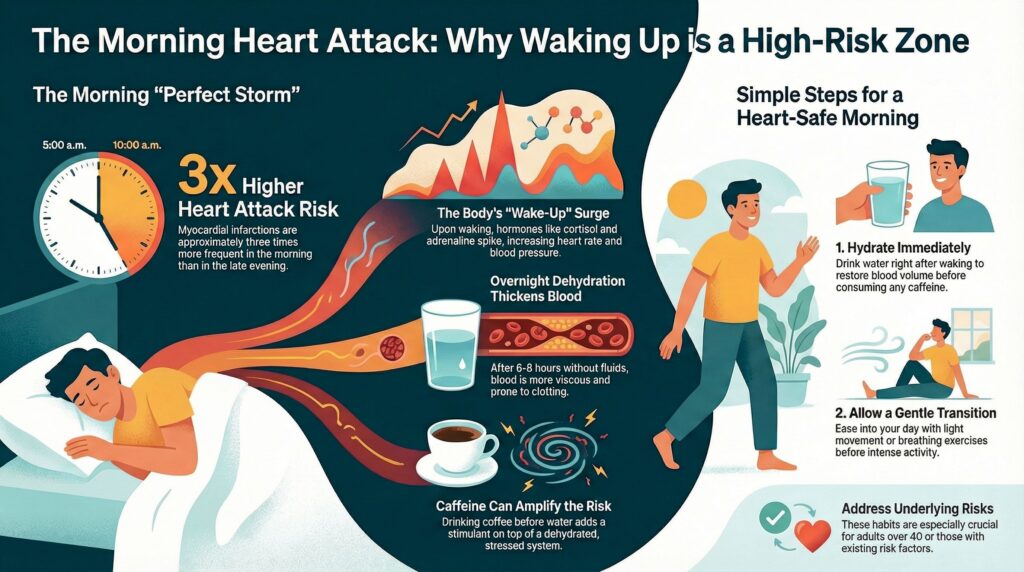
The Morning Cardiovascular Transition
When we wake up, the body undergoes a rapid autonomic nervous system shift. During sleep, the parasympathetic nervous system predominates, supporting repair, recovery, and vascular relaxation. Upon waking, the sympathetic nervous system activates to prepare us for movement, alertness, and action.
This transition triggers:
- A sharp rise in cortisol
- Increased release of epinephrine and norepinephrine
- Elevations in heart rate and blood pressure
- Increased vascular tone and vasoconstriction
These changes are normal and necessary. However, in susceptible individuals, they create a vulnerable cardiovascular window.
Morning Dehydration and Blood Viscosity: Most people wake up dehydrated. After six to eight hours without fluid intake, plasma volume is reduced. This leads to:
• Increased hematocrit
• Increased blood viscosity
• Greater platelet aggregation
• Reduced blood flow through small vessels
In practical terms, the blood is thicker and more prone to clotting in the morning than at almost any other time of day. When thicker blood encounters narrowed or inflamed arteries, particularly in the setting of underlying atherosclerosis or endothelial dysfunction, the risk of clot formation and plaque rupture rises significantly.
The Overlooked Habit That Amplifies Risk
One of the most common morning habits is reaching for coffee or other stimulants immediately upon waking, often before any hydration.
Caffeine increases sympathetic nervous system activity, raises catecholamines, transiently elevates blood pressure, and promotes vasoconstriction. When combined with dehydration and the natural morning cortisol surge, this can further increase vascular resistance and blood viscosity at precisely the wrong time.
This does not mean coffee causes heart attacks. Nor does it mean caffeine is inherently harmful. The issue is timing and physiological context. Layered onto a dehydrated state, sympathetic activation, and preexisting cardiovascular risk, this habit may meaningfully amplify the morning danger window.
Why This Matters More After 40
As we age, vascular elasticity decreases, endothelial function declines, and inflammatory burden increases. Men over 40, in particular, are more likely to have:
• Subclinical atherosclerosis
• Insulin resistance
• Hypertension
• Sleep apnea or nocturnal hypoxia
• Increased inflammatory markers
All of these factors magnify the effects of morning vasoconstriction and hypercoagulability. In this context, small daily behaviors can have outsized long-term consequences.
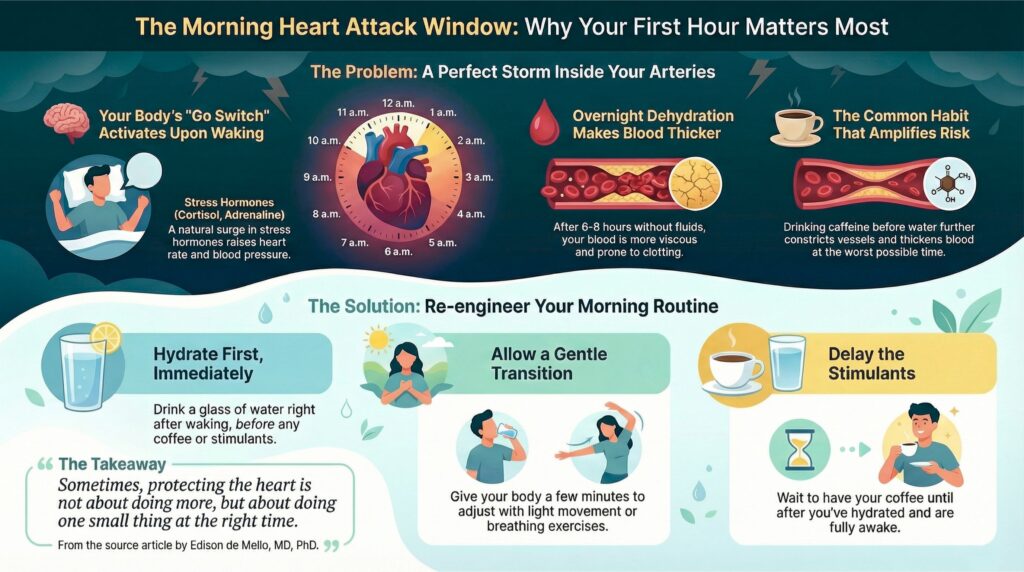
A Preventative, Functional Perspective
From an integrative and preventative standpoint, reducing morning cardiovascular risk does not require extreme interventions. It requires respecting physiology.Simple strategies include:
- Hydrating immediately upon waking, before caffeine
- Allowing a brief transition period with light movement or breathing
- Delaying stimulants until hydration and circulation are restore
- Addressing sleep quality and screening for sleep apnea
- Monitoring inflammatory markers, insulin resistance, and blood viscosity-related risks
These steps do not replace diet, exercise, stress management, or lipid optimization. They complement them.
The Bigger Takeaway: Morning heart attacks are not caused by one hidden habit alone. They occur at the intersection of dehydration, autonomic nervous system shifts, blood viscosity, vascular tone, and underlying cardiometabolic risk.
Understanding this intersection allows us to move from fear-based messaging to intelligent prevention. Sometimes, protecting the heart is not about doing more, but about doing one small thing at the right time.
Recent Peer-Reviewed Studies and Scientific Statements
- A 2025 scientific statement from the American Heart Association emphasizes the importance of circadian rhythms in cardiometabolic health (blood pressure regulation, hormonal balance, metabolic control, risk factors) and notes that disruptions to these rhythms are linked to cardiovascular disease risk. (American Heart Association)
- A 2025 study published in Nature identified molecular mechanisms (BMAL1–HIF2A interaction) that explain time-of-day differences in heart attack severity. Morning onset was associated with worse outcomes in preclinical models, pointing to underlying circadian biology in ischemic injury. (ScienceDaily)
- A 2025 narrative review in the European Heart Journal confirms that myocardial infarctions occur more frequently in the morning (approximately threefold higher than late evening), and that circadian influences on platelet aggregation and blood pressure contribute to this pattern. (OUP Academic)
- A 2025 review in Circulation Research describes how circadian regulatory systems (internal clocks) influence cardiovascular events such as heart attack and sudden cardiac death, and highlights therapeutic opportunities such as chronotherapy (timing-based treatment). (PubMed)
- A 2025 case–control study in Journal of Medical Internet Research reports associations between circadian rhythm disruption (including sleep irregularities) and increased incidence and mortality from myocardial infarction, reinforcing the role of timing and biological rhythms in cardiovascular risk. (JMIR)
- Harvard Health and expert commentary from 2025 summarize state-of-the-art reviews linking the body’s internal clock to heart-attack timing, blood pressure surges, clotting tendencies, and circadian misalignment from behaviors like shift work and irregular sleep. (Harvard Health)
About the Author:
Edison de Mello, MD, PhD, is a board-certified integrative physician and psychotherapist, and founder of the Akasha Center for Integrative Medicine and Akasha Naturals. He’s passionate about a patient-centered approach, “Meeting the patient before meeting their diseases.” Dr. de Mello is the author of Bloated: How to Eat Without Pain and also serves on non-profit boards that promote health, wellness, and community well-being.

















